Hospital outreach to the community: repercussion on sepsis morbidity and mortality
Keywords:
Sepsis/complications; Minors.Abstract
Introduction: sepsis constitutes a worldwide health problem with high morbodity and mortality rates; any training effort would contribute to the decrease in mortality.Objective: to determine the repercussion on sepsis morbidity and mortality for Pepe Portilla Children´s Hospital in Pinar del Río, after the hospital outreach into primary health care.
Material and method: a quantitave, descriptive, longitudinal and prospective research was carried out from June 1st 2010 to June 30th 2011, of infants at ages 1-18 months admitted to the intensive care service as being disagnosed with sepsis.
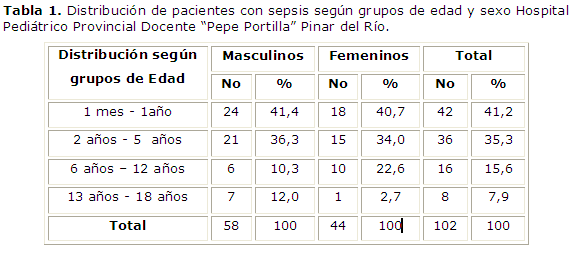
Results: 41.2% of the infants were under one year, before the hospital outreach 60% of the them were admitted in advanced stages, then 55.9% of the patients entered the sepsis stage and only 33.5% entered the serious stage. 18.8% of early stages cases had natural history under 24 hours and in the 75% of the cases were detected 72 hours after the onset of symptoms. After the hospital outreach, 56.3% arrived in early stages, diaognosis is made before the 24 hours.
Conclusions: after the hospital outreach to the community, sepsis managment and septic shock, the early diagnosis increased, with an increase in infant mortality rate.
Downloads
References
1. Lescay Cantero M. Sepsis y empleo de antimicrobianos en las unidades de cuidados intensivos polivalentes. Rev Acta Médica 2011;13(1):76-82
2. Aguirre Tejedo A, Echarte Pazos JL, Mínguez Masó S, Supervía Caparrós A, Skaf peters E, Campodarve Botet I. Implementación de un "Código Sepsis Grave" en un servicio de urgencias. España. Emergencias [Internet] 2009 [citado 12 May 2012];21(4): [aprox. 13 p.]. Disponible en: http://www.semes.org/revista/vol21_4/4.pdf
3. Levy J H. Treating Shock- Old Drugs, New Ideas. N Engl J Med 2010;362(9):841-843.
4. Singhia S, Khilnanib P, Lodhac R, Santhanamd I, Jayashreea M, Ranjite S, Ramachandranf B, Alig U, Sachdevh A, Chughh K, Udanii S,Uttamj R, Deopujarik S, Kissoonl N. Guidelines for treatment of septic shock in resource limited environments. Journal of Pediatric Infectious Diseases 2009;4:173-192.
5. Dellinger RP, Levy MM , Carlet JM, Bion J, Parker MM , Jaeschke R, et-al. Surviving Sepsis Campaign:International guidelines for managementof severe sepsis and septic shock: 2008. Intensive Care Med 2008; 34:17-60
6. Downie L, Armiento R, Subhi R,Kelly J, Clifford V, Duke T. Community-acquired neonatal and infant sepsis in developing countries: efficacy of WHO's currently recommended antibiotics—systematic review and meta-analysis. Arch Dis Child 2013;98:146-154
7. González Velásquez A, Valdés Armas F, Fernández Reverón F, Ardisana Cruz O, Álvarez González AI, Francisco Pérez JC. Comportamiento de la sepsis en terapia intensiva pediátrica. Revista Cubana de Medicina Intensiva y Emergencias. [Internet]. 2007 [citado 20 May 2011]; 6(3): Disponible en: http://bvs.sld.cu/revistas/mie/vol6_3_07/mie08307.htm
8. Crespo Barrios A, Cruz Alvarez Canto I, Alvarez Montalvo D. Mortalidad por Sepsis en UCIP. Hospital Pediátrico Juan Manuel Márquez 2002-2005. IV Congreso Internacional URGRAV 2006. Ciudad de La Habana: Cuba; 2006.
9. Daniels R, Nutbeam T. ABC of Sepsis. Edicion first. USA: Blackwell; 2010.
10. Montalván GL. Epidemiología de la sepsis en una unidad de cuidados intensivos pediátricos. Estudio de 5 años. Habana: XXVl Congreso Nacional de Pediatría; 2008.
11. Montalván González GL, López Torres O, Berdalles Milián JD. Conocimientos y percepción sobre la sepsis en pediatría. Rev. Med. Electrón.? [revista en la Internet]. 2009? Dic [citado? 2013? abril 09] ;? 31(6): Disponible en: http://scielo.sld.cu/scielo.php?script=sci_arttext&pid=S1684-18242009000600004&lng=es.
12. Dellinge RP, Levy MM, Andrew Rhodes MB; Annane D, Gerlach H, Opal SM, et al. Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012. Critical Care Medicine 2013;41(2):580-637.
13. Arriagada D, Díaz F, Donoso A, Cruces P. Clasificación PIRO en sepsis grave y shock séptico pediátrico: Nuevo modelo de estratificación y su utilidad en pronóstico Rev Chil Infect 2010;27(1):17-23.
14. Montalván González GL. Shock séptico en pediatría: un acercamiento a su manejo. Rev Cubana Pediatr? [revista en la Internet]. 2008? Mar [citado? 2013? Abr? 03];? 80(1). Disponible en: http://scielo.sld.cu/scielo.php?script=sci_arttext&pid=S0034-75312008000100008&lng=es
15. Russell JA. How much fluid resuscitation is optimal in septic shock? Critical Care 2012; 16:146.
16. Bayer O, Reinhart K, Kohl M, Kabisch B, Marshall J, Sakr Y, Bauer M, Hartog C, Schwarzkopf D, Riedemann N. Effects of fluid resuscitation with synthetic colloids or crystalloids alone on shock reversal, fluid balance, and patient outcomes in patients with severe sepsis: A prospective sequential analysis. Crit Care Med 2012; 40(9): 2543-2551.
17. Pastrana Román Irene, Corrales Varela Ariel Iván, Quintero Pérez William, Rodríguez Rodríguez Mariela, Álvarez Reinoso Sarah. Estrategia de capacitación en atención primaria y emergencias hospitalarias. Indicadores de calidad en sepsis. Rev Ciencias Médicas? [revista en la Internet]. 2012? Jun [citado? 2013? Abr? 18];? 16(3): 120-138. Disponible en: http://scielo.sld.cu/scielo.php?script=sci_arttext&pid=S1561-31942012000300012&lng=es
18. Sistema de Vigilancia Epidemiológica del Síndrome de Respuesta Inflamatoria Sistémica en las UTIP. Departamento Nacional Programa Materno Infantil Reunión Metodológica PAMI. Habana; 2011.
Published
How to Cite
Issue
Section
License
Authors who have publications with this journal agree to the following terms: Authors will retain their copyrights and grant the journal the right of first publication of their work, which will be publication of their work, which will be simultaneously subject to the Creative Commons Attribution License (CC-BY-NC 4.0) that allows third parties to share the work as long as its author and first publication in this journal are indicated.
Authors may adopt other non-exclusive license agreements for distribution of the published version of the work (e.g.: deposit it in an institutional telematic archive or publish it in a volume). Likewise, and according to the recommendations of the Medical Sciences Editorial (ECIMED), authors must declare in each article their contribution according to the CRediT taxonomy (contributor roles). This taxonomy includes 14 roles, which can be used to represent the tasks typically performed by contributors in scientific academic production. It should be consulted in monograph) whenever initial publication in this journal is indicated. Authors are allowed and encouraged to disseminate their work through the Internet (e.g., in institutional telematic archives or on their web page) before and during the submission process, which may produce interesting exchanges and increase citations of the published work. (See The effect of open access). https://casrai.org/credit/


